
NURSING HOME SAFETY DURING COVID: PPE SHORTAGES
Seven months into pandemic, 20 percent of facilities lacked enough supplies
Thousands of nursing homes nationwide are dealing with horrific shortages of masks, gowns and other items they need to protect residents, workers and the broader community from COVID-19. And seven months into this pandemic, the shortages have actually become much worse.
Downloads
Maryland PIRG Foundation and Frontier Group

Thousands of nursing homes nationwide are dealing with horrific shortages of masks, gowns and other items they need to protect residents, workers and the broader community from COVID-19. And seven months into this pandemic, the shortages have actually become much worse.
At any given time, about 1.3 million people with long-term medical issues or short-term rehabilitation needs are residing in the nation’s 15,000 nursing homes. And too many of them are at risk, according to an analysis of government data by U.S. PIRG Education Fund and Frontier Group.
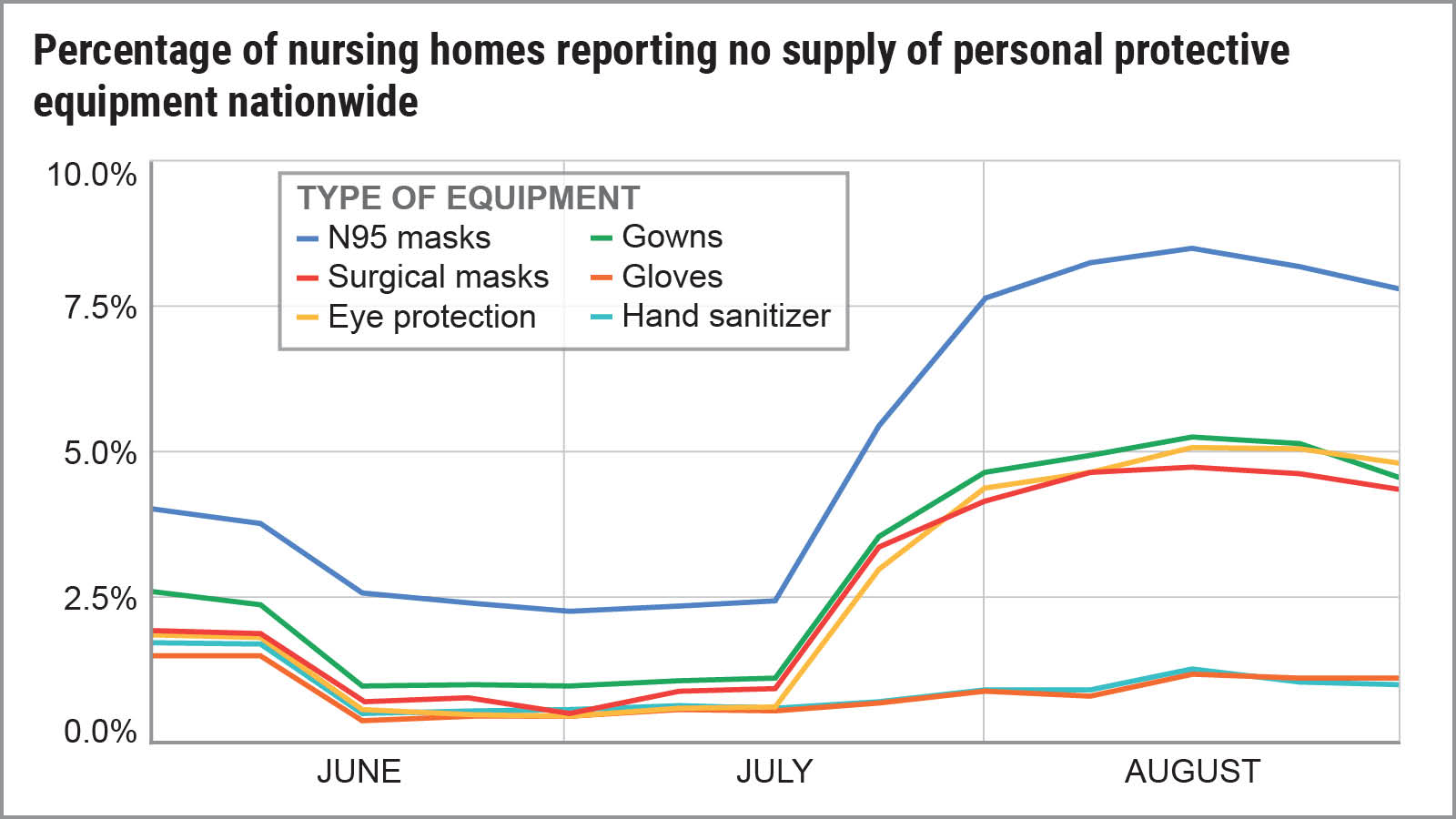
Source: U.S. PIRG / Frontier Group analysis of data from data.CMS.gov
As of late August, 226,495 residents in 2,981 nursing homes nationwide were at risk because the homes had dangerously low supplies of one or more types of personal protective equipment (PPE) such as N95 masks or gowns, according to data submitted to the federal government. That means that 20 percent of nursing homes in late August had a less-than-one-week supply of one or more types of PPE, which represents a critical shortage by industry standards.
The shortages actually became more grave as the summer went on, with three times as many nursing homes reporting they were completely out of masks, gowns and eye protection in late August, compared with mid-July.
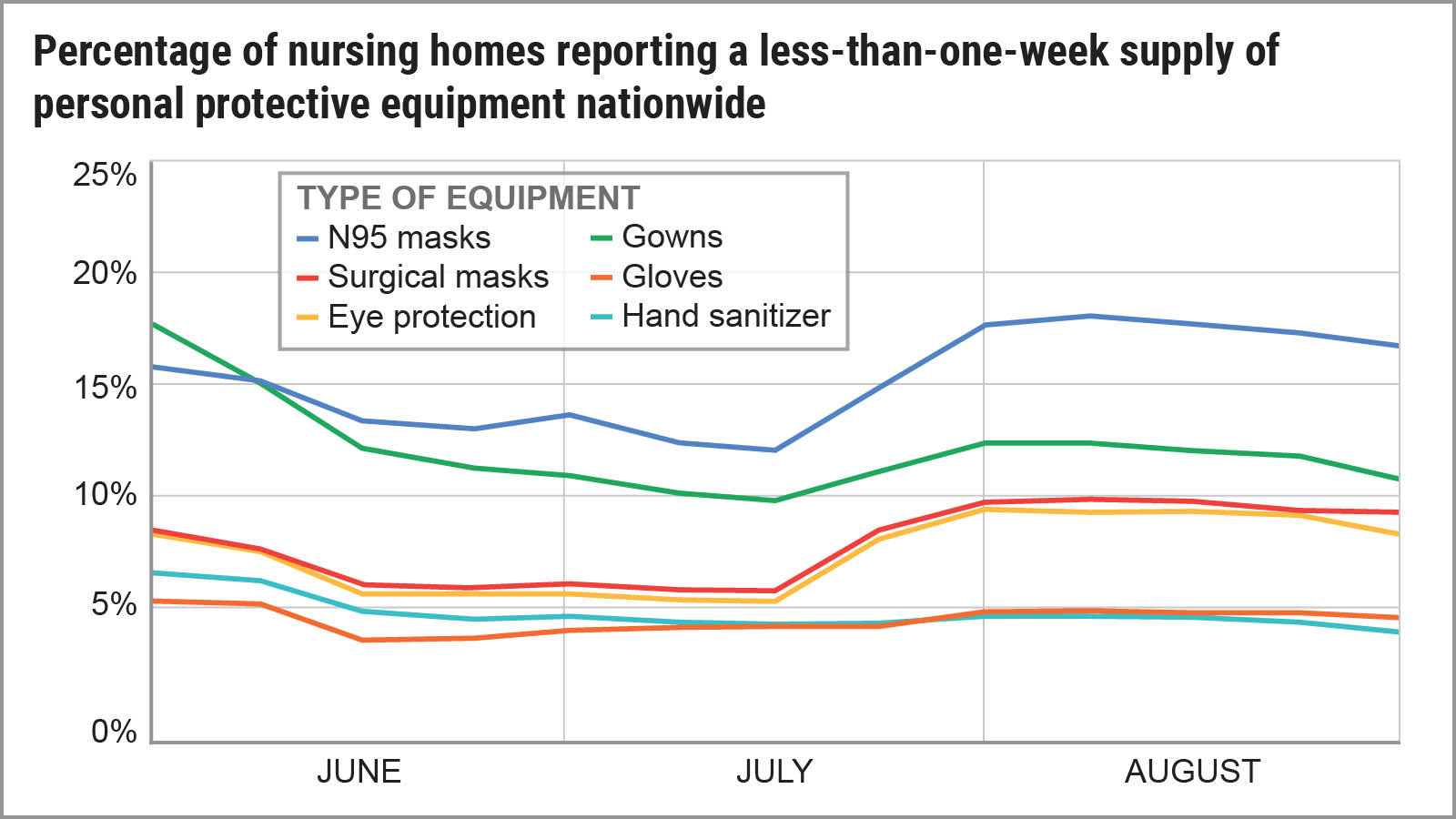
Source: U.S. PIRG / Frontier Group analysis of data from data.CMS.gov
Forty-six percent of all nursing homes nationwide reported they didn’t have a one-week supply of at least one type of PPE at some point from May through August. A one-week supply is considered the minimum acceptable. If a home has an outbreak, it can burn through its limited supply in a day or two. In addition, a home may have no idea when its next shipment of PPE may arrive. Homes with less than one week’s supply often ration, forcing workers to re-use PPE or go without.
In January, the U.S. government declared a public health emergency in response to the global threat from the coronavirus. Yet seven months after the public health emergency declaration, this nation was still experiencing dangerous shortages of PPE.
Heightened danger in nursing homes
It’s not entirely surprising that while nursing homes contain less than one-half of 1 percent of the U.S. population, they’ve produced 3 percent of the nation’s COVID-19 cases and 27 percent of deaths.
Experts believe nursing homes have been hit harder in part because the living space is tighter, residents are there around-the-clock, and people in nursing homes and rehabilitation facilities are generally older and in poorer health than the overall population. Certainly, the PPE shortages have made difficult situations even worse.
Workers are generally expected to change their PPE before every new patient to avoid potentially transferring the coronavirus from one patient to another.
“The consequences are devastating,” said Dr. David Gifford, chief medical officer at the American Health Care Association/National Center for Assisted Living (AHCA/NCAL), the nation’s largest industry association. “Long-term care is not a profession where social distancing is possible — caregivers must closely interact with their patients and residents to provide the utmost care.”
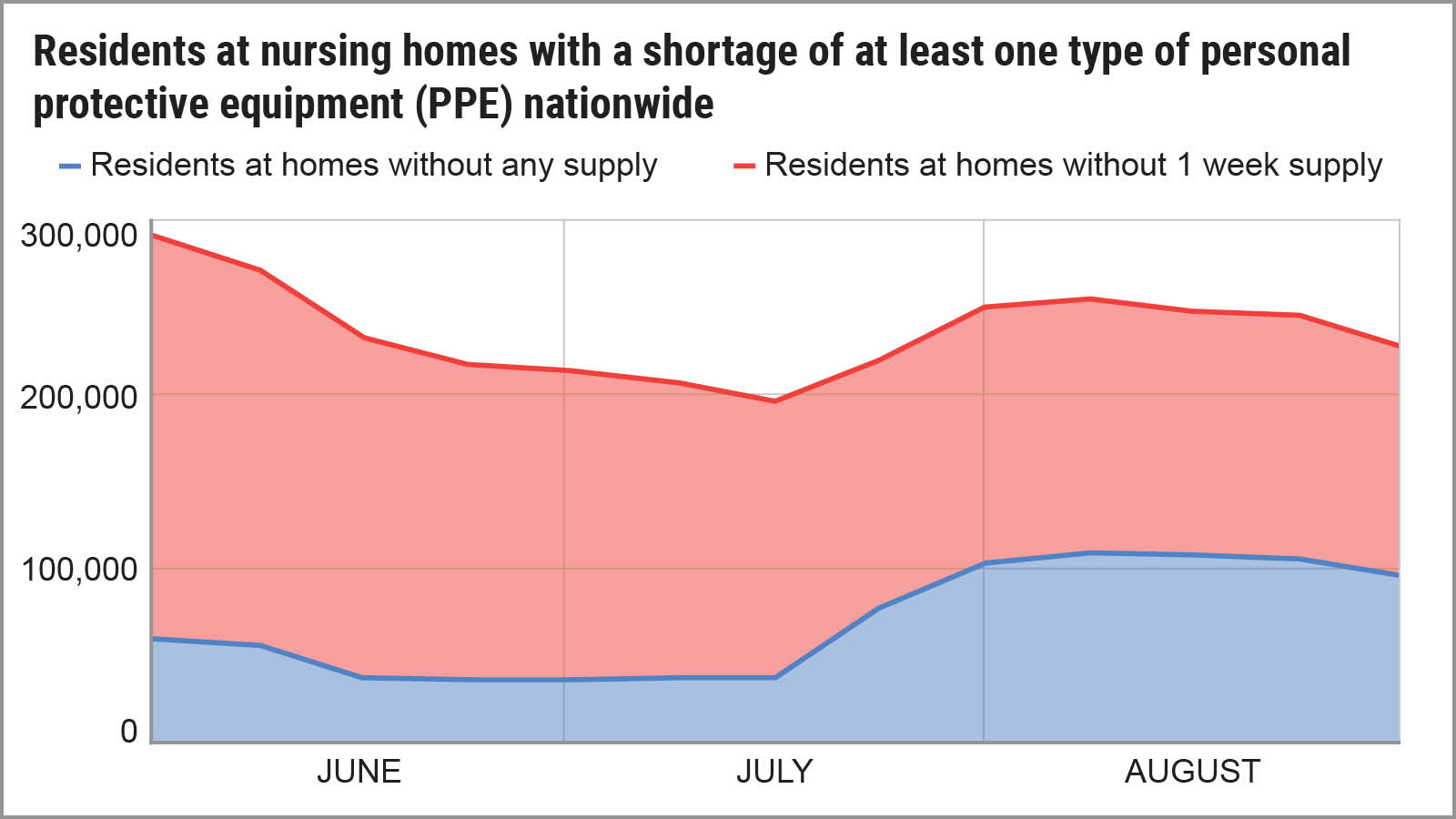
Source: U.S. PIRG / Frontier Group analysis of data from data.CMS.gov
The impact of PPE shortages? It goes beyond putting individual patients at risk. Experts say:
- Outbreaks can and do occur rapidly in a setting such as a nursing home.
- Workers go home and can spread the virus to family members or to others in the community when they go to the grocery store, church or other public places.
- Workers can get sick and be unable to work, or be exposed and need to quarantine. Either of these can cause staff shortages.
- Even if workers aren’t getting sick, they’re getting stressed.
- Stressed workers are at more risk of illness. And stressed workers, especially aides and others who may earn barely more than minimum wage, are more likely to quit.
What’s behind the shortages?
It’s clear the nation as a whole didn’t have adequate amounts of PPE to handle a once-in-a-century global pandemic. (No explanations have been provided about why the Strategic National Stockpile under the U.S. Department of Health and Human Services didn’t have more supplies.)
Nursing homes usually buy PPE individually through third-party suppliers, the AHCA said. But the supply chain has been completely disrupted this year. “During this pandemic, providers were desperate for PPE, creating their own or even trying to buy it off Amazon,” Gifford said.
Overall, the shortages were more severe in some states because of myriad reasons: outbreaks, economics, poor planning, politics or some combination of those.
Why is the situation so bad in nursing homes?
Demand for PPE is coming from every sector of the economy, not just health care. The world supply chain was strained. The AHCA begged the federal and state governments to help nursing homes and assisted living centers, Gifford said. But long-term care facilities weren’t prioritized to receive PPE, he said.
Robyn Grant, director of public policy and advocacy at the nonprofit National Consumer Voice for Quality Long-Term Care, said the U.S. government didn’t provide much help: a two-week supply of PPE. In addition, a number of facilities reported that some of the PPE was defective, including gowns with no arm holes and expired N95 masks, Grant said.
As bad as it was in the spring, it got worse, with PPE shortages skyrocketing in nursing homes in mid-July. Experts blame three phenomena: the reopening of restaurants and other businesses in many states in June and July; outbreaks in the South as people flocked to vacation spots and started enjoying summer fun; and the resumption of activities within other medical businesses such as elective surgeries, in-person doctor’s appointments and veterinary procedures.
The PPE shortages exist across various health care settings, according to the American Nurses Association (ANA), which in September released a survey of 21,000 nurses nationwide. Forty-two percent of them said they continue to cope with “widespread or intermittent” shortages of PPE.
PPE shortages in nursing homes put residents and staff at greater risk of getting the virus and spreading it, Grant said.
“We have heard staff say that they have been required to use one mask for days, and that in some cases they have had to use garbage bags because there weren’t enough gowns,” she said. “We’ve also heard staff talk about how worried they are about taking the virus back home to their loved ones.” Reusing a mask violates health care protocols.
This crisis isn’t going away without action
We face the possibility of a brutal fall and winter if another wave of COVID-19 combined with a normal flu season further strains PPE supplies. Three months ago, a 25-member commission of non-partisan experts, organized by the Centers for Medicare & Medicaid Services, issued urgent warnings that the problem will become more dire. In its updated report in September, the Coronavirus Commission on Safety and Quality in Nursing Homes said homes continue to be plagued by shortages in PPE, as well as testing and staffing shortages.
“Additional federal action is necessary to ensure sufficient availability of high-quality testing and PPE,” the commission wrote. “Without this, and related training, the virus will continue to spread.”
Here’s what’s needed:
- Full use of the Defense Production Act to increase U.S. production of PPE.
- Passage of the Medical Supply Transparency and Delivery Act, which was introduced in Congress in the spring, to improve the supply chain so it’s centralized and transparent. This would also help keep prices stable because states, individual health care facilities, school systems and businesses wouldn’t be competing against each other for supplies.
- In the absence of federal coordination, states need to find their own solutions, including forming multi-state consortiums for regional supply chains, so they’re not competing against each other for the same PPE, tests and equipment.
- Money in a new COVID relief bill to help nursing homes.
- The federal and state governments to prioritize getting PPE to providers coping with severe shortages.
Something must change soon. “Our health care heroes are risking their own safety and security to continue their valiant work of caring for our nation’s most vulnerable,” Gifford said. “And we must rally around them and our vulnerable residents.”
Topics
Find Out More


NURSING HOME SAFETY DURING COVID: CASES & VACCINES

Nursing home safety during COVID: Cases and Vaccines
